Encouraging Early detection
Breast cancer with an early diagnosis has a better chance of being cured:
Breast cancers that are found quickly are usually at an early stage and require less aggressive treatment than more advanced cancers.
- Some screening tests can even detect cancer while it is still in the pre-cancerous stage. This means that it can be treated before it becomes cancerous.
- Half of the tumors discovered via early detection are less than 2 cm in size.
- In these cases, since the cancer is caught early, it has less time to spread and is easier to treat.
- Advanced breast cancers require more aggressive treatment, over a longer period.
- Early detection can, in some cases, prevent the need for chemotherapy.
Many women are alive today because their cancer was detected early.
- For breast cancer treated at an early stage, the five-year survival rate is 99%.
- In the last 20 years, the Quebec Breast Cancer Screening Program (QBCSP) has prevented 7 out of 1,000 deaths in Quebec.
- The QBCSP aims to reduce the breast cancer mortality rate by 25% among women aged 50 to 69.
Convincing reasons for screening tests!
All the reasons listed below show the importance of having a screening mammogram every two years (if you are between 50 and 69 years of age) and of regularly observing your breasts.
Your doctor may advise you to have screening mammograms before the age of 50 or more frequently in these cases:
- You’ve had breast cancer before.
- You’ve had biopsies that have detected breast changes, such as abnormal non-cancerous cells (atypical hyperplasia).
- You have a family history of breast cancer, especially if your mother, sister or daughter was diagnosed before menopause or if there are inherited mutations in the BRCA1 or BRCA2 genes.
Researchers are working to find new, reliable and non-invasive methods for early detection of breast cancer.
For instance, biomarkers, which are molecules that indicate disease, are being investigated for early detection.
Studies are evaluating the possibility of detecting various cancers using blood samples. This technique would make screening simple and fast.
Since cancer cells can be found in the blood of cancer patients, several research groups are trying to develop techniques to detect them effectively in people who have not been diagnosed.
One promising approach is called CancerSEEK, which consists of detecting cancer cells and mutated DNA circulating in the blood. At present, the average prediction rate for all types of cancer is 82%, but only 33% for breast cancer. Researchers are still working to improve this test’s sensitivity. In addition to finding cancer while it is still at an early stage, this method would be useful for monitoring the cancer’s progress and adapting treatments accordingly.
Cohen JD et al. “Detection and localization of surgically resectable cancers with a multi-analyte blood test,” Science, published online January 18, 2018.
Cancer cells secrete metabolites, organic molecules that are unique to these cells. Researchers in Copenhagen have shown that metabolites in the blood can predict the appearance of any kind of cancer two to five years in advance. Analysis of metabolites published in a 2015 study of 800 women predicted the appearance of cancer in 80% of cases. In comparison, mammography has a success rate of 75%.
Gene analysis could be used to determine women’s level of risk of developing breast cancer. In fact, 180 genetic mutations are known to be linked to a higher possibility of developing breast cancer. Having just one mutation increases the risk very little; it is the combination of several mutations that influences the probabilities. To develop new tests for early detection, researchers are working to determine which genetic profiles are most at risk. It is estimated that this could identify up to 10 times more at-risk women, who could be monitored more closely so that any cancer would be detected and treated at an early stage. It should be noted that the proportion of high-risk women is low, but it is still important to detect them early.
The Rose Ages Breast Health Centre at the Ottawa Hospital is working to improve breast cancer diagnosis with three-dimensional mammography. This technique would improve early detection by allowing a more in-depth examination of tissue. It is thought that it would discover 30% more cancer and reduce the number of false-positive diagnoses. This technique is currently under investigation.

What are diagnostic tests?
After an abnormality is detected, further tests are conducted to confirm or rule out the presence of breast cancer. If cancer is found, it will be analyzed to determine its status and characteristics.
Breast Cancer diagnostic tools
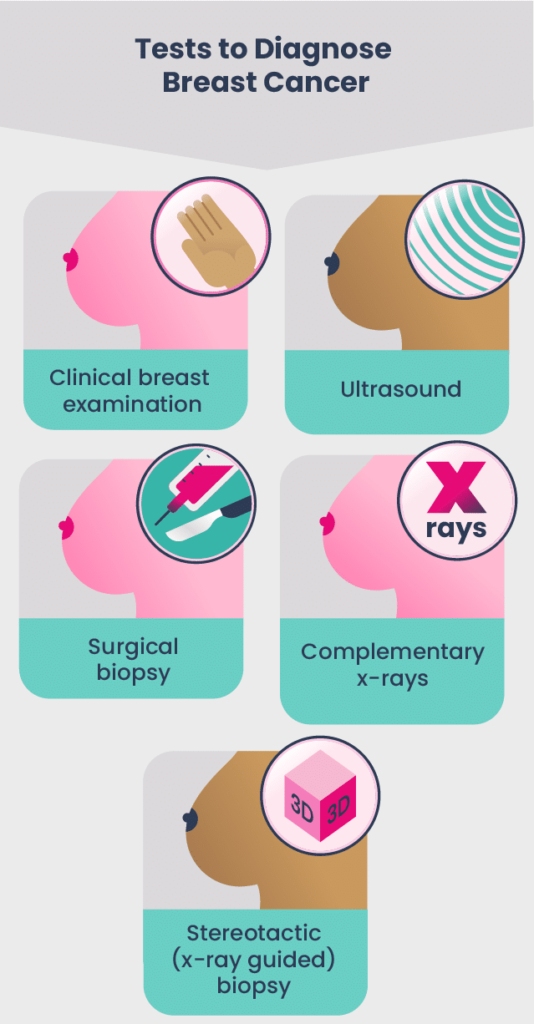
The following are the main tests, other than screening mammograms, that provide an accurate diagnosis of breast cancer:
- Additional X-rays: Mammograms, called scintimammography, are used to better define the nature of the lesion.
- Ultrasound: This examination is used mainly to determine whether there are cysts in the breast.
- Non-surgical biopsy: Cells or tissue are removed using different types of needles.
- Surgical biopsy: Surgery is used to remove part of the lesion.
- Stereotactically-guided biopsy: In this computer-assisted procedure, a wire is inserted into a non-palpable lesion. The wire very precisely guides the surgical sampling from the lesion.
Diagnostic mammography is performed on women who have already detected a sign of breast cancer, such as a lump or abnormal breast tissue. This detection may have been made by the women themselves during breast observation, by a physician during a clinical breast examination, or by a screening mammogram. A diagnostic mammogram is more thorough and a little longer than a screening mammogram, and it takes more detailed images from different angles.
Breast ultrasound projects high-frequency sound waves onto the solid parts of the body without penetrating them.
Healthy breasts consist of soft tissue or liquid, while tumours are solid masses, which are revealed by breast ultrasound. A doctor may recommend this type of test to:
- Examine any mass or abnormality detected by a clinical breast exam or mammogram
- Determine whether an abnormality is a solid tumor or a fluid-filled cyst
- Properly identify the problem area of the breast prior to biopsy
How is a breast ultrasound performed?
This test can be done in a doctor’s office, at a clinic, in a hospital or in an outpatient setting. Depending on the case, this examination should be expected to take between 15 and 30 minutes, sometimes longer.
The woman lies down on an ultrasound table, and a technician applies a lubricating gel to the skin on the area to be examined. This gel improves the transmission of sound waves. A healthcare professional will then gently slide a transducer, which is a microphone-like probe, directly on the skin. The high-frequency sound waves emitted by the transducer are reflected as echoes, which a computer analyzes and then uses to produce images on a screen.
In general, women can go on with their normal daily activities after a breast ultrasound, since this test does not require anesthesia and does not cause side effects or pain.
In addition to breast ultrasound, other techniques can be used to obtain images of the tumour in the breast and indicate its progress, in particular to find out whether the cancer has spread to other parts of the body. Generally, these tests do not require anesthesia and do not cause pain.
X-rays are among a wide range of techniques used to image the breasts, including computed tomography (CT), galactography, scintimammography, bone scan, magnetic resonance imaging (MRI). In addition, ultrasound or X-rays may be taken of organs other than the breasts. Click here to learn more about any of these imaging techniques.
More specifically, magnetic resonance imaging (MRI) is an examination that uses radio waves and a powerful magnetic field to see contrasts within tissue. There are some contraindications, but no harmful effects are known. MRI is mainly used to detect the presence of metastases and to inform the choice of treatment.
Only a breast biopsy can definitively diagnose cancer. This procedure consists of taking a sample of cells or tissues from the breast(s) or the lymph nodes and examining them in the laboratory, where the presence or absence of cancerous cells can be confirmed.
A breast skin biopsy may also be performed if inflammatory breast cancer is suspected, while a nipple biopsy may be performed if Paget’s disease is suspected.
The doctor will choose which of the existing breast biopsy types to use, depending on the breast abnormality that has been detected. Some biopsies require imaging techniques and local or general anesthesia, while others do not.
When a biopsy contains cancer cells, more detailed laboratory analyses of the samples are often required to better understand the breast cancer status and to plan the best possible treatment. The main laboratory tests available include visualization of the cells, assessment of the rate of proliferation by measuring ki-67 expression, analyzing the tumour hormone receptor status, HER2-gene test, genetic analysis of the cancer cells and blood work.

In some cases, blood work may be necessary to check the amount and appearance of different types of blood cells. The results can provide information on whether or not breast cancer is present and, if it is, how the disease is progressing and spreading to the rest of the body. This then informs the doctor about whether the patient’s organs are functioning normally.
The section below provides an overview of the methods that may be used, by describing each procedural option. The healthcare team will decide which strategy is best for each woman based on her circumstances.
Sentinel node biopsy involves finding and removing a sentinel node to check for cancer cells. The sentinel node is the first in a chain of lymph nodes, and is the first to receive and filter out cancer cells.
Before the sentinel node is biopsied, a low-level radioactive substance (a radiotracer) is injected. This substance is carried through the lymphatic system, allowing the surgeon to see the lymph nodes and find the sentinel node. This type of biopsy is simpler than an axillary lymph node biopsy and has fewer side effects.
Axillary lymph node removal (also known as axillary dissection or axillary lymph node dissection) involves removing axillary lymph nodes from the armpit. It make it possible to:
– Evaluate whether cancer cells are present in the axillary nodes (number of affected nodes, number of cells per node), to know the scope of the cancer
- Remove the nodes containing cancerous cells
- Remove the nodes if there is a high risk of the cancer spreading
- Reduce the risk of recurrence
The surgeon makes an incision under the arm and removes between 10 and 40 lymph nodes, which are then analyzed by a pathologist.
A small drain and drainage bag are put in place after the excision to catch any fluid from the operated area and to promote healing. The drain remains in place for a few weeks or until the flow diminishes. Patients may return home one or two days after surgery. You may experience side effects such as infection, fluid build-up under the skin near the incision, swelling, stiffness, difficulty moving the arm or shoulder, numbness or pain. A build-up of lymph in the soft tissue can cause lymphedema.


